Introduction
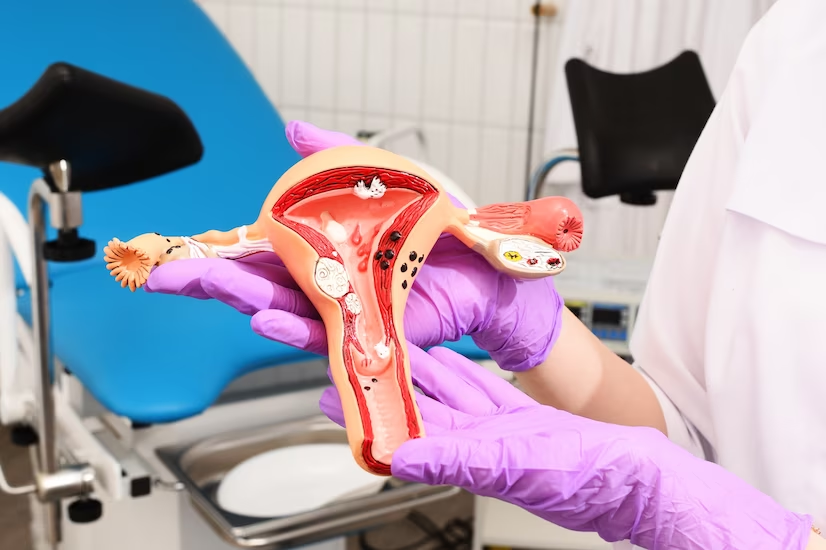
Absolute Uterine Factor Infertility (AUFI) is a type of fertility disorder where the absence or dysfunction of the uterus makes conception and maintaining a pregnancy impossible. This condition impacts approximately 1 in 500 women of reproductive age and accounts for around 8% of infertility cases in couples. Women experiencing AUFI due to congenital conditions such as Rokitansky-Kuster-Hauser syndrome or Hysterectomy can only fulfil their desire to become mothers through “Surrogacy.” However, surrogacy is prohibited in many countries. Medical research has explored Uterus Transplants (UTx) as a potential alternative for these patients. After numerous animal testing and clinical trials spanning several decades, several successful pregnancies have been carried to full term using UTx.1,2.
Blessing for Women Devoid of a Uterus
Uterus transplantation involves transplanting a healthy uterus from a living or deceased donor into a woman who lacks a functional uterus, enabling her to conceive and carry a child to term. This procedure presents a unique opportunity for women born without a uterus, who had their uterus removed for medical reasons, or who had an irreparable uterine condition.3
For these women, the possibility of becoming pregnant and experiencing childbirth through this innovative procedure represents a life-changing opportunity. Uterus transplantation promises to empower aspiring mothers to experience the joys and challenges of pregnancy, birth, and motherhood like any other woman.3
The Transplantation Procedure2
Before the Surgery
- Before proceeding with the transplant procedure, the patient will undergo a comprehensive evaluation to assess their suitability.
- Various diagnostic and screening tests will be conducted to evaluate their physical and psychological health.
- If deemed eligible, the female’s or donor’s eggs and a sperm sample from the male partner or donor will be collected.
- Fertilization of these eggs with sperm will take place in a laboratory to create healthy embryos. Concurrently, the potential uterine donor will undergo a series of tests to ensure their compatibility for donation.
During the Surgery
- The initial phase of the transplant procedure involves the donor’s hysterectomy, which typically lasts around 8 hours.
- There are different approaches for this step, such as Robotic Hysterectomy (laparoscopic), where the uterus is removed through five small incisions, or an Open Hysterectomy, where the surgeon makes a long vertical incision from the belly button to the pubic hairline to extract the uterus.
- The patient will be admitted to the hospital on the scheduled surgical day.
- The transplant procedure, carried out under general anaesthesia, will take approximately 4 to 6 hours.
- Post-surgery, the patient will be initially transferred to the intensive care unit (ICU) and then to a recovery room for a minimum of 5 to 7 days.
 After the Surgery
After the Surgery
- A uterine transplant necessitates a minimum of three months for the healing process.
- The patient will be on immunosuppressive medications throughout the pregnancy and until the hysterectomy is successful.
- Approximately 4 to 6 weeks after surgery, menstruation is expected to begin. Subsequently, the fertilized egg (embryo) will be transplanted into the patient’s uterus under controlled laboratory conditions.
- The patient will be advised to rest and adhere to the necessary guidelines after the embryo has been implanted into the uterine wall.
- In the event of a successful pregnancy, the patient will deliver the baby via C-section at the end of the gestation period.
- Depending on their preference for future children, patients may choose to undergo a hysterectomy along with the C-section or defer it for later.
Challenges and Ethical Considerations
While uterus transplantation shows immense promise, it is not without its challenges and ethical considerations. The procedure itself is overly complex and demands surgical expertise and precision. Rejection of the transplanted organ by the recipient’s immune system is a significant concern, leading to a requirement for lifelong immunosuppressive medication.1,3.
Moreover, the availability of suitable donors is a critical issue. Living donors must undergo a significant physical and psychological evaluation, and their willingness to undergo the procedure is a rare occurrence. The use of deceased donors presents an opportunity to expand the pool of potential donors, but it also poses ethical questions regarding the procurement process and consent.2
Conclusion
As a relatively new approach, uterus transplantation continuously advances through ongoing research endeavors. These studies focus on improving the technique, boosting success rates, and mitigating complications. Furthermore, advancements in immunosuppressive therapy are set to increase the procedure’s safety and accessibility.
Uterus transplantation is a game-changing advancement in the field of assisted reproductive medicine. This innovation holds the potential to fulfil the desires of numerous hopeful mothers by enabling them to experience pregnancy and childbirth. As medical knowledge expands and technology evolves, the accessibility and safety of uterus transplantation are expected to increase, delivering a glimpse of hope for those seeking motherhood.
Nevertheless, it remains imperative to address ethical considerations and medical challenges comprehensively. This approach ensures that the remarkable developments made in this field maintain their safety and inclusivity, serving the needs of all deserving women.1,2,3.
References
- Benjamin P Jones, Niccole Ranaei-Zamani, Saaliha Vali, et al. Options for acquiring motherhood in absolute uterine factor infertility; adoption, surrogacy, and uterine transplantation. The Obstetrician & Gynaecologist. April 2021; 23(2):138–147. DOI: 10.1111/tog.12729.
- Andrea Etrusco, Manuela Fabio, Gaspare Cucinella et al. The reproductive potential of uterus transplantation: Future prospects. ACTA BIOMEDICA. April 2022; 93(2): e2022138. DOI: 10.23750/abm.v93i2.12868
- Saso S, Clarke A, Bracewell-Milnes T, et al. Psychological Issues Associated with Absolute Uterine Factor Infertility and Attitudes of Patients Toward Uterine Transplantation. Progress in Transplantation. March 2016;26(1):28-39. DOI: 10.1177/1526924816634840