In metabolic health, the equilibrium of blood glucose, lipids, blood pressure, and body mass index (BMI) within the healthy range is considered a cornerstone. While conventional wisdom dictates that lifestyle choices are pivotal in maintaining metabolic health, recent research suggests a novel perspective—specifically, the influence of reproductive milestones, particularly in women, including conditions like Polycystic Ovary Syndrome (PCOS).
This article explores the intersection of metabolic health, lifestyle, and reproductive factors, shedding light on the complexities that shape an individual’s susceptibility to metabolic dysfunction.
The Basics: Metabolic Health and Syndrome
A person who boasts optimal blood glucose levels, favorable lipids, normal blood pressure, and a healthy BMI is deemed metabolically healthy. However, those diverging from this healthy spectrum face the ominous threat of metabolic syndrome—a cluster of conditions that significantly elevate the risk of coronary heart disease, type 2 diabetes, stroke, and various other health complications. Shockingly, one in three adults in the United States grapples with metabolic syndrome, underscoring the urgency for a comprehensive approach to metabolic well-being.
Traditional Wisdom and the National Heart, Lung, and Blood Institute
Guided by the venerable National Heart, Lung, and Blood Institute, healthcare professionals have long championed the pillars of metabolic health. Choosing heart-healthy foods, maintaining an ideal weight, regular physical activity, stress management, sufficient sleep, and bidding farewell to smoking are heralded as the fundamental tenets for safeguarding against heart disease and thwarting the onset of type 2 diabetes.
A Paradigm Shift: Reproductive Milestones and Women’s Metabolic Health
In a groundbreaking departure from convention, recent research has illuminated a previously underappreciated facet of metabolic health—the impact of reproductive milestones, particularly in women. While lifestyle factors have traditionally dominated discussions, this new review suggests that characteristics tied to reproductive milestones may wield a significant influence on a woman’s vulnerability to metabolic dysfunction, potentially paving the way for conditions such as type 2 diabetes and high cholesterol.
Screening for Reproductive Risk Factors: Polycystic Ovary Syndrome (PCOS)

The researchers behind this transformative review propose a paradigm shift in the approach to women’s metabolic health. Beyond lifestyle considerations, they advocate screening reproductive risk factors as an initial step in preventing and treating metabolic diseases. This includes scrutinizing elements such as early onset of menstruation, polycystic ovary syndrome (PCOS), weight gain during pregnancy, and the severity of menopause symptoms.
Unlocking the Evidence: Reproductive Milestones and Metabolic Health

The review delved into the intricate connections between reproductive milestones and metabolic health, uncovering compelling links that span a woman’s lifetime:
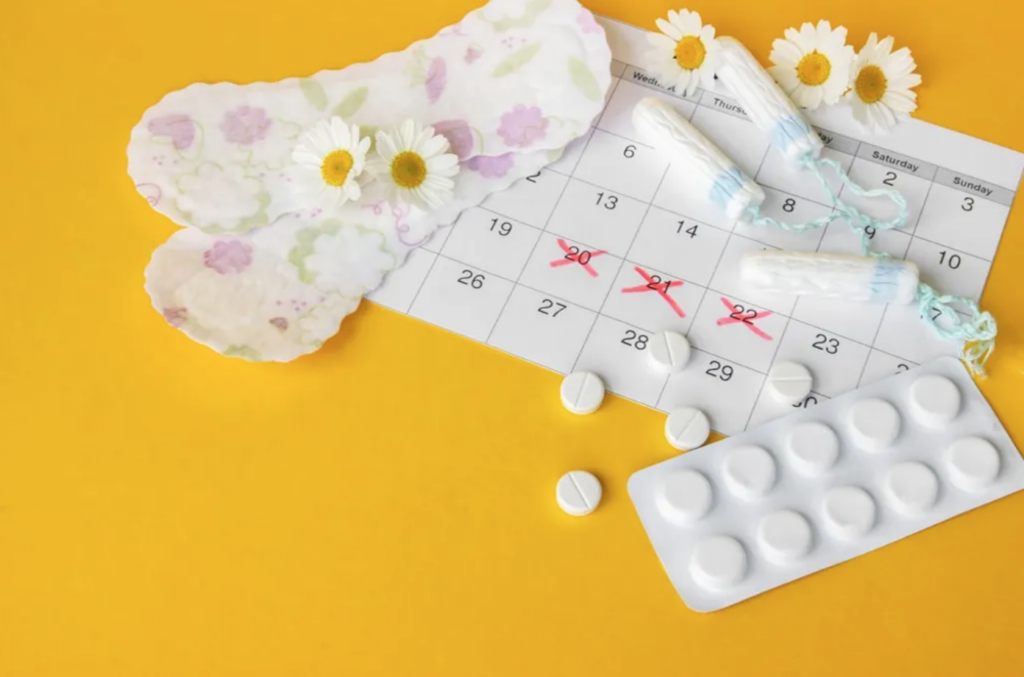
- Early Menarche: Initiating menstruation before the age of 12 was associated with abnormal blood glucose levels, high cholesterol, metabolic syndrome, and type 2 diabetes.
- Irregular Menstruation: Chronic irregular menstruation proved to be a red flag, elevating the risk of developing type 2 diabetes compared to regular menstrual cycles.
- PCOS: A robust relationship emerged between Polycystic Ovary Syndrome (PCOS), obesity, and type 2 diabetes, emphasizing the intertwined nature of reproductive and metabolic factors.
- Pregnancy-related Factors: From gestational diabetes to excessive weight gain during pregnancy and elevated gestational lipid levels, these factors were all linked to poorer metabolic health in later life.
- Lactation: Longer lactation periods were associated with improved metabolic health and a reduced risk of type 2 diabetes and metabolic syndrome.
- Menopause: Severe menopause symptoms and early menopause were correlated with a heightened risk of type 2 diabetes. Encouragingly, evidence suggested that postmenopausal estrogen therapy could mitigate this risk.
The Common Thread: Insulin Resistance
While the research refrained from exploring causation, a recurring theme emerged—most identified risk factors are intertwined with increased insulin resistance. Dr. G. Thomas Ruiz, a distinguished board-certified OB/GYN, concurred and highlighted that conditions like above-average weight gain in pregnancy, PCOS, and gestational diabetes are all associated with insulin insensitivity, adding complexity to the metabolic equation.
Conclusion
As we navigate the multifaceted landscape of metabolic health, integrating reproductive milestones into our understanding heralds a new era in personalized healthcare. Beyond the traditional realms of lifestyle choices, clinicians must now consider the nuanced impact of a woman’s reproductive journey on her metabolic well-being. By acknowledging and addressing these unique risk factors, healthcare professionals can further tailor interventions, enhancing the effectiveness of preventive measures and treatments. In this evolving paradigm, collaboration between practitioners, researchers, and individuals is pivotal, ensuring a holistic and personalized approach to metabolic health.
Reference
Irregular periods, PCOS linked to higher risk of diabetes, high cholesterol [Internet]. Accessed on February 07, 2024. Medical News Today. Available from: https://www.medicalnewstoday.com/articles/irregular-periods-pcos-linked-to-higher-risk-of-diabetes-high-cholesterol
About Docquity
If you need more confidence and insights to boost careers in healthcare, expanding the network to other healthcare professionals to practice peer-to-peer learning might be the answer. One way to do it is by joining a social platform for healthcare professionals, such as Docquity.
Docquity is an AI-based state-of-the-art private & secure continual learning network of verified doctors, bringing you real-time knowledge from thousands of doctors worldwide. Today, Docquity has over 400,000 doctors spread across six countries in Asia. Meet experts and trusted peers across Asia where you can safely discuss clinical cases, get up-to-date insights from webinars and research journals, and earn CME/CPD credits through certified courses from Docquity Academy. All with the ease of a mobile app available on Android & iOS platforms!