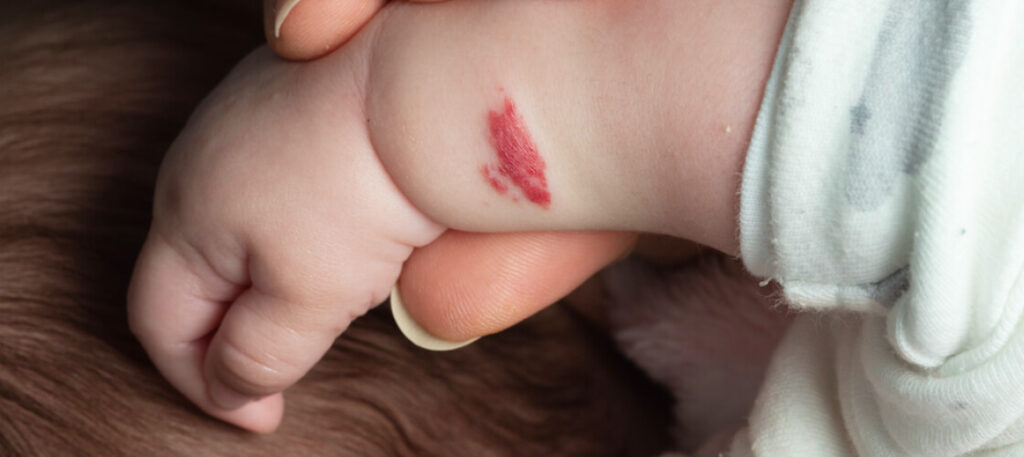
Infantile hemangiomas (IHs) are the most common type of benign tumors in childhood and affect 4-5% of infants.1 While most are small and don’t require treatment, others are more severe and may cause scarring, disfigurement, functional impairment, ulceration, and other abnormalities.1 The following clinical practice guidelines (CPG) by the American Academy of Pediatrics (AAP) are useful for primary care providers and pediatricians and provide a robust framework for management and clinical decision-making.1
Highlights of the clinical practice guidelines
Key action statement 1A
“Clinicians should classify an IH as high risk if there is evidence of or potential for the following: (1) life threatening complications, (2) functional impairment or ulceration, (3) structural anomalies (e.g., in PHACE syndrome or LUMBAR syndrome), or (4) permanent disfigurement (grade X, strong recommendation).”1
This statement allows for the timely identification of the IHs that would benefit from early intervention.1 Two significant challenges associated with IH are disease heterogeneity and distinctive growth of IHs.1 Yet, it is essential to identify and treat some IHs early to avoid risk of disfigurement, complications, etc. The following are indications that may necessitate a more detailed look or require early treatment:1
- Life-threatening complications
- Ulceration or the risk of ulceration
- Functional impairment or the risk of functional impairment
- Risk of distortion of landmark points or permanent scarring
- Evaluation for identifying significant associated structural anomalies
Key action statement 1B
“After identifying an IH as high risk, clinicians should facilitate an evaluation by a hemangioma specialist as soon as possible (grade X, strong recommendation).”1
Ensuring timely evaluation by a specialist is essential since high-risk IHs must be treated as early as possible to prevent complications.1 This statement highlights the need for this since it is critical to take advantage of the time period to intervene and avoid delays. Research has shown that IHs appear as early as infancy and many typically form before 4 weeks.1 High-risk IHs should be identified as soon as possible and referred to a hemangioma specialist.1
Key action statement 2A
“Clinicians should not perform imaging unless the diagnosis of IH is uncertain, there are 5 or more cutaneous IHs, or associated anatomic abnormalities are suspected (grade B, moderate recommendation).”1
Since the majority of IHs can be diagnosed clinically, imaging is not typically required.1 However, imaging may be used for diagnosis if the lesions are distinct or grow inconsistently or unexpectedly.1 Additionally, healthcare professionals may use noninvasive imaging to monitor the success of treatment and management, but this is not usually required.1 Imaging is also recommended if there is risk of PHACE or LUMBAR syndromes.1 The type of imaging recommended is abdominal ultrasonography.1 If five or more IHs are present, clinicians may screen for hepatic IH.1 Abdominal ultrasonography detects hepatic IHs 95% of the time and avoids ionizing radiation and sedation, making it the ideal imaging method.1
Key action statement 2B
“Clinicians should perform ultrasonography as the initial imaging modality when the diagnosis of IH is uncertain (grade C, weak recommendation).”1
When IH diagnosis is uncertain, ultrasonography with Doppler imaging may be used since this avoids exposure to ionizing radiation, which may be dangerous for young infants.1 Additionally, it avoids sedation.1 Doppler ultrasonography can be used for both monitoring and screening for hepatic IHs.1
Key action statement 2C
“Clinicians should perform MRI when concerned about associated structural abnormalities (e.g., PHACE syndrome or LUMBAR syndrome) (grade B, moderate recommendation).”1
Some infants may be at risk of PHACE or LUMBAR syndromes, making it important to perform imaging for associated structural anomalies.1 MRI is the best imaging modality for this since it provides contrast and shows vascular components and anatomy.1 While MRI may require sedation, it avoids ionizing radiation.1 It’s critical to note duration because prolonged exposure may negatively affect brain development in children younger than 3 years.1
While spinal ultrasonography and Doppler ultrasonography may be used for this purpose, an MRI will eventually be required for the definition it provides, making it the optimal choice.1 It’s important to note that computer tomography is not considered because it involves ionizing radiation.1
Key action statement 3A
“Clinicians should use oral propranolol as the first-line agent for IHs requiring systemic treatment (grade A, strong recommendation).”1
Clinical guidelines for management include using oral propranolol for IHs that need systematic treatment.1 This is the treatment of choice and was approved by the U.S. Food and Drug Administration (FDA) in March 2014.1 Research has shown the effectiveness of oral propranolol to be 95%, which is higher than other interventions, including steroids, bleomycin, and pulse-dye laser (PDL).1
Key action statement 3B
“Clinicians should dose propranolol between 2 and 3 mg/kg per day unless there are comorbidities (e.g., PHACE syndrome) or adverse effects (e.g., sleep disturbance) that necessitate a lower dose (grade A, moderate recommendation).”1
The general consensus for dosing propranolol is 2-3 mg/kg per day.1 It’s important to note that evidence-based recommendations on dosing twice or thrice daily are not available.1 However, both the FDA and European Medicine Evaluation Agency recommend dosing twice daily.1
This is not a rigid recommendation since dosing may need to be adjusted in certain cases. For example, those suffering from PHACE syndrome will need dosage adjusted to prevent an increased risk of stroke.1 Those with progressive IH ulceration and those experiencing side effects will also need adjusted doses.1 High-risk patients should start with the lowest effective dose and adjust accordingly.1 It’s recommended that oral propranolol be administered thrice daily to avoid fluctuations in blood pressure.1
Key action statement 3C
“Clinicians should counsel that propranolol be administered with or after feeding and that doses be held at times of diminished oral intake or vomiting to reduce the risk of hypoglycemia (grade X, strong recommendation).”1
It’s critical that oral propranolol be taken with feeds to avoid hypoglycemia and hypoglycemia-induced seizures.1 Infants and young children are especially at risk, making it essential to educate caregivers on the importance of administering oral propranolol during or immediately after feeding.1 Since hypoglycemia can be avoided by ensuring administration during or after feeding and adequately educating caregivers, routine glucose screening is not necessary.1 It’s also important to educate parents and caregivers about the dangers of prolonged fasting, since this can result in hypoglycemia and vomiting.1 Eight or more hours of fasting results in an increased likelihood of hypoglycemia in infants and young children.1
Key action statement 3D
“Clinicians should evaluate patients for and educate caregivers about potential adverse effects of propranolol, including sleep disturbances, bronchial irritation, and clinically symptomatic bradycardia and hypotension (grade X, strong recommendation).”1
While hypoglycemia is one of the risks associated with incorrect use of oral propranolol, it’s not the only one. Parents and caregivers should be informed about other risks, including cold extremities, sleep disturbances, bronchial irritation, gastrointestinal symptoms, and decrease in blood pressure or heart rate.1
Key action statement 3E
“Clinicians may prescribe oral prednisolone or prednisone to treat IHs if there are contraindications or an inadequate response to oral propranolol (grade B, moderate recommendation).”1
This statement underscores the use of corticosteroid therapy for infants who cannot tolerate β-blocker therapy.1 It may also be used when β-blocker therapy is ineffective or contraindicated.1 Since corticosteroids were the standard of care before oral propranolol, this is an effective treatment option.1
Key action statement 3F
“Clinicians may recommend intralesional injection of triamcinolone and/or betamethasone to treat focal, bulky IHs during proliferation or in certain critical anatomic locations (e.g., the lip) (grade B, moderate recommendation).”1
Some IH subsets may benefit from the use of intralesional corticosteroid injections.1 This is both safe and effective and is most useful for small and localized IHs which increase bulk and threaten anatomic landmarks.1 It is not recommended for larger IHs because of the increased volume of steroids used and other complications resulting from this.1
Key action statement 3G
“Clinicians may prescribe topical timolol maleate as a therapy for thin and/or superficial IHs (grade B, moderate recommendation).”1
Topical timolol may be useful in managing superficial or thin IHs and have been used for pediatric glaucoma for decades.1 Research has shown the treatment to be effective and have minimal side effects, making this a more popular treatment for thin and superficial IHs.1 Furthermore, research on young infants has shown that early treatment with topical timolol inhibits IH growth.1
That being said, healthcare professionals should be cautious since timolol is more potent than propranolol and avoids first-pass liver metabolism.1 This is especially the case when more than 1 drop twice daily is prescribed or if this treatment is used for young or preterm infants.1
Key action statement 4
“Clinicians may recommend surgery and laser therapy as treatment options in managing selected IHs (grade C, moderate recommendation).”1
Surgery and laser treatment can be used to treat certain IHs but healthcare professionals opt for these less frequently in favor of β-blocker therapy.1 Surgical intervention is not usually performed in infancy because of higher risk of complications and the use of anesthetics.1 Additionally, results are superior when growth has ceased, especially for IHs on the nasal tip or lip.1
However, early surgical intervention is a favorable option when IHs obstruct or deform important structures or involve sensitive areas when it comes to aesthetics.1 If lesions do not improve with pharmacotherapy or wound care, are well-localized, and will make later reconstruction easier, surgery is considered a good option.1 Surgery is also recommended when resection will be necessary down the line and scars would be similar, and when IHs leave residual skin changes.1
In the majority of cases, surgery is best avoided until at least three years of age.1 Most surgical interventions take place between 3 and 5 years because the lesions may resolve themselves, the tumor will be smaller, making the surgery easier and the scar smaller, and because the surgery may be safer if the IH consists of adipose tissue instead of blood vessels.1 Since IHs do not improve greatly after 3-4 years, it’s unnecessary to wait beyond this age.1
PDL may also be used to treat IHs but is not as effective as other interventions since it only penetrates the superficial dermus.1 As a result, it may aid in reducing redness, but does not affect the deeper elements of the IH.1 While PDL is used to treat ulcerations, the evidence for this is scarce and comes from small cases and case reports.1 Additionally, propranolol is more effective than PDL, making it a better choice.1
Key action statement 5
“Clinicians should educate parents of infants with an IH about the condition, including the expected natural history, and its potential for causing complications or disfigurement (grade X, strong recommendation).”1
This statement highlights the importance of educating parents about IH.1 The guidance and education should be specific to the child’s IH and should ease parental anxiety when the IHs are non-problematic.1 Additionally, education informs parents about signs to note in case there are any changes.1 In addition to being informed about the growth period, it’s important to encourage parents to schedule visits or share photographs for reassessment should changes occur.1 Parents should be informed about involution age and residual changes such as scars.1
When IHs are problematic, parents or caregivers should be urged to consult hemangioma specialists in a timely manner to seek early intervention.1
Conclusion
There are a number of challenges associated with implementing these CPGs, including IHs’ dynamic nature, the difficulty to predict IHs in infants, and no techniques to reliably predict growth.1 However, these CPGs are especially useful since they highlight the importance early identification and outline best practice and evidence-based treatment options.1 Pediatricians and other healthcare professionals can benefit from these guidelines to ensure optimal care for IH.
References
- Krowchuk DP, Frieden IJ, Mancini AJ, et al. Clinical Practice Guideline for the Management of Infantile Hemangiomas. Pediatrics. 2019;143(1):e20183475.
- doi:10.1542/peds.2018-3475